Introduction and Background
Because of the impending shortages of laboratory personnel, a consortium of laboratory partners including multiple education and industry members, applied for and received a Department of Labor (DOL) grant through St. Paul College: Developing Capacity to Grow Minnesota’s Clinical Laboratory Workforce. There were a variety of projects associated with this grant, but all were essentially focused on significantly increasing graduation rates of qualified medical laboratory personnel for the state’s workforce. However, the common issue facing us was the limited availability of required clinical education placements. Even before increasing our educational programs’ enrollments it was getting harder and harder to find the appropriate quality clinical placements for students. But with the approaching drastic increase in the number of students needing clinical placements, we had to find a new way to provide the “clinical” for our students, to ease the impact on the clinical sites and focus the time in the clinical site to only those skills that we could not teach on campus.
To find a solution for our students and for the clinical sites we looked away from historical models. What did we need our clinical sites to be able to provide and what had we already taught them on campus? We realized that instead of the traditional clinical internship where bench instructors teach students all of the testing methods from scratch, we needed a clinical experience for our students. As you can imagine, this change away from the traditional concept of clinical training was initially difficult for both academic and clinical faculty to accept. We needed to work extensively with our clinical affiliates to develop a concept of what we needed in this partnership. However, since we have clinical affiliates throughout the state (one-third outside the metro area) and into the neighboring states, we needed a way to reach all of these hospital and clinic locations without extended travel for university faculty and time away from work for clinical personnel (Figure 1).
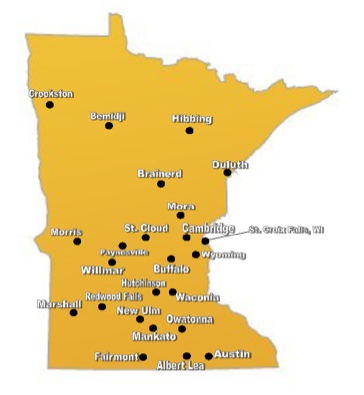
Figure 1:Non-Metro Clinical Training Sites
How could this be accomplished in a timely and consistent manner? We investigated the option of delivery of this information electronically including a web-based approach for preceptor in-service orientation and education. But we were not sure that the clinical personnel who were used to an in-person face-to-face interaction would accept this alternative delivery. We decided to explore three components of delivering an orientation and program specific information to our clinical affiliation sites: online introduction modules, web-conferencing, and the use of a course management system as a repository for relevant materials.
Development of DOL Modules
As part of the Department of Labor (DOL) grant, an online interactive Preceptor Training module was developed along with a companion module for students. The module for Preceptor Training was an extension of the orientation. Screen-by screen module content was developed by our program faculty using PowerPoint® or Microsoft Word®. These screens were then converted to Adobe® Flash by a contracted programmer. This individual also had some experience in instructional design and acted as a reviewer for flow and understanding of the content. The purpose of each module was to provide an overview understanding of this new model of clinical training, how and why this model integrated with our curriculum and with the outcomes expected for accreditation. The modules were designed with an awareness that students and preceptors would go through both modules while preparing for the clinical experience. Each section contains interactive Knowledge Checks to reinforce the stated objectives and the student module also contains Observation Checks where students are asked to observe aspects of their clinical site.
The preceptor training module we developed consists of seven sections. The Introduction describes the rationale for the new model of a clinical experience including our history as a profession, current economic pressures, and the value of clinical education. “Roles and Definitions” describes the interactive roles and responsibilities of the students, clinical preceptors, academic and clinical coordinators during the clinical experience. “What Is Entry Level?” help preceptors understand that they are not training a new employee to become fully-proficient on their hospital’s instruments, but are exposing students to the culture, environment and workflow of the clinical laboratory as well as the laboratory’s role in patient care. “Student Affective Domain” discusses the need to describe and define the professional behaviors that are part of the medical culture. So often we forget that these are things we need to teach to the students along with the laboratory science. “Creating A Positive Environment” stresses the need to maintain a positive atmosphere for learning and to provide guidance for students so they can improve their performance. We know how difficult this can be considering the levels of stress typically found with laboratory work. The section on “Student Evaluations” describes the preceptors' responsibilities for providing a quality evaluation on student competencies including the need for constructive feedback as well as encouragement. The “Summary” section refers the preceptors to their Education Coordinator or academic affiliate for additional information.
The comparable student orientation module, called "What To Expect On Your Clinical Experience," was designed to help students understand their responsibilities during the clinical experience. The module contains four sections and begins with ”Before You Begin” which reminds them of the need to prepare for this portion of their education. Students are told to plan ahead in finding the location, parking, and determining whether there are additional requirements for that site such as a site-specific orientation. "How the Laboratory Works" follows the path of a patient’s sample through the hospital from drawing the blood to reporting out the patients’ results, describing these functions in a small clinic setting as well as a large urban medical center hospital. “A Typical Day” follows a fictitious student through a day during her clinical experience, including her interactions with fellow students who are in other laboratory sections and the preceptors. “Making the Transition” describes how students can begin to make the transition from college student to a practicing laboratorian. Part of the clinical experience is the development of laboratory professionals who can exhibit mature interpersonal relationships and appropriate communication skills, adhere to the highest standards of the profession, and exhibit confident and mature use of health care knowledge and skill. Students may enter the profession with competent communication, organizational and ethical skills but need to learn how to apply them to the healthcare setting.
Web-Conferencing Sessions
Although the modules were helpful as an introduction to the clinical experience concept, we needed to provide a more in-depth and specific in-service for the preceptors through a series of web conferences to explain our curriculum in each sub-discipline of CLS. The web conferences utilized a university meeting system that provided two-way audio conferencing along with Internet displays. We needed to use separate teleconference design for audio discussions due to fire-wall security issues at some clinical sites. This provided a synchronous meeting format for clinical sites, especially those at considerable distance from our campus location. It also removed the need for travel and provided consistency in the information delivered to our clinical sites.
We first held a number of sessions where program faculty presented a discipline specific overview of didactic content and student laboratory activities along with a discussion of overall expectations for the clinical experience. Each Course Director outlined the lecture material and student laboratories in a PowerPoint presentation that was uploaded to the Web conference platform. The sessions concluded with a summary of expectations for rotations in light of what was presented. Because most of our clinical training sites take students from many different college program designs, they were not really aware of the extent and depth of our on-campus instruction. These teleconference and web-based conference sessions utilizing UMConnect and GopherConferencing provided the opportunity for campus faculty to have direct discussions with the preceptors in each discipline. The ability to answer questions immediately and to address any concerns from the clinical sites garnered a lot of support for our new model along with constructive feedback for on-going improvement. A second set of web-conferences were designed for all disciplines which focused on preceptor behaviors and student evaluations processes during the clinical experience. These discussions were then incorporated into the final modules in the online course site.
Course Management System (CMS)
To make all of these materials available to the preceptors, we developed courses within our university Moodle CMS. One course was developed exclusively for clinical site personnel that included access to the DOL training modules, ready access to handouts and other materials from the web conferencing sessions, evaluation forms and instructions. Other sites were developed for students which included access to the DOL modules and other general materials they would need for their clinical experience such as checklists and evaluation forms. The student CMS site also contained resources for students such as information about housing if they were assigned to non-metro sites. Rather than printing out and providing each student with a packet of information the Moodle site acted as a repository for all of the materials they might need while in their clinical training. The student sites also contained addresses, directions, and contact information for their clinical assignment as well as links to hospital specific policies and other requirements. Preceptors and students completed their evaluations through the CMS system creating a paperless process. Since the CMS also contains email and chat capabilities it provided a mechanism for enhanced communication between the program and our clinical affiliates as well as with students. This was particularly helpful since our program has students at many locations throughout the region including a large number of non-metro sites. Students and preceptors both quickly became comfortable using this method of interactive communication.
Preceptor Survey
As part of our on-going program evaluation we wanted to know if our new model was still reaching our program goals for our graduates. We invited all conference and clinical site members to participate in an online survey at the end of the 2011 session. The survey gathered demographics about the preceptors including age, practice level, number of years in the profession and number of years teaching at the bench. We also asked about their satisfaction with the DOL modules, web-conferencing, and CMS Moodle course sites.
Of the 130 individuals involved in our clinical experience for students 73 completed the survey (56%). Twenty three of the respondents attended the live web-conferences. Those that did not participate in the live sessions were either unaware of the offering or they were not able to get away from work to attend the live sessions. Of those responding, all felt that the web conferences (live or recorded) were helpful in explaining their role as a preceptor and increased their knowledge regarding our expectations for our new clinical experience.
The DOL modules, Moodle CMS site and Web Conferences were an efficient means of providing in-service training and communicating with our clinical sites. This was a cost effective use of time and finances minimizing extended travel for university faculty and time away from work duties for hospital personnel.
Lessons Learned
- Because of security limitations at some of our hospital clinical sites we were unable to use UM Connect as the sole process for web conferencing. Personnel using hospital computers have limited access to some programs and web sites. We did not anticipate this issue initially but adjusted by using GopherConference teleconference for the audio portion of the in-service sessions.(Figure 2)
- Some locations had electronic interference during the live chats but were able to access the recorded sessions easily.
- Clinical personnel easily became adept at use of the Moodle CMS. They liked the centrally located repository of forms and information as well as its 24/7 access.

Figure 2:Clinical Training Settings
As part of the DOL grant criteria, the preceptor and student training modules are available for free public use through our program web site.
Acknowledgement
This product was partially funded by a grant awarded to St. Paul College under the President’s Community-Based Job Training Grant as implemented by the US Department of Labor’s Employment and Training Administration (COL SGA/DFA PY-07-01). The information contained in this product was created by a grantee organization and does not necessarily reflect the official position of the U.S. Department of Labor. All references to non-governmental companies or organizations, there services, products, or resources are offered for information purposes and should not be construed as an endorsement by the Department of Labor. This product is copyrighted by the institution that created it and is intended for individual organizational, noncommercial use only. http://cahp.umn.edu/CLS